7 min read
Safety in Healthcare: 17 Recommendations for Healthcare Organizations
Performance Health Partners
July 15, 2022

Even though increasing efforts have been made over the past two decades, safety in healthcare remains a major area of concern. Experts have in recent years identified numerous evidence-based best practices shown to be effective in harm reduction, yet they are infrequently implemented successfully across organizations. Improving safety and reducing preventable adverse events necessitates a collaborative, consistent, and coordinated effort by all stakeholders.
Safety in Healthcare: Shifting Toward Total Systems Safety
According to the National Steering Committee for Patient Safety (NSC), thousands of fragmented patient safety initiatives are in place in individual organizations or collaborations across the United States and around the world. As a result, our healthcare system still fails a percentage of patients, families, and healthcare workers. The key to reducing preventable patient harm is adopting total systems safety.
Achieving total systems safety demands a shift from reactive, fragmented interventions to a proactive approach in which risks are anticipated and addressed through system-wide safety processes established and applied across the entire health care continuum. It also involves coordination at several levels, which subsequently requires collaboration among all involved stakeholders.
Without the same support, respect, resources, and attention given to patients’ safety, providers and personnel can’t fulfill their potential and/or are “more likely to fail to follow safe practices, not work well in teams, and make errors,” according to the Institute for Healthcare Improvement (IHI).
In their “Safer Together: A National Action Plan to Advance Patient Safety” report, IHI highlights the insights of the organizations represented on the NSC. It was created based on the NSC members’ collective determination to change the status quo around preventable harm and safety in healthcare to provide actionable recommendations and clear tactics.
The NSC created this plan with the understanding that healthcare organizations are at different points in their progress toward creating safer care, and with the knowledge that its recommendations would have to apply across different settings, specializations, and populations served.
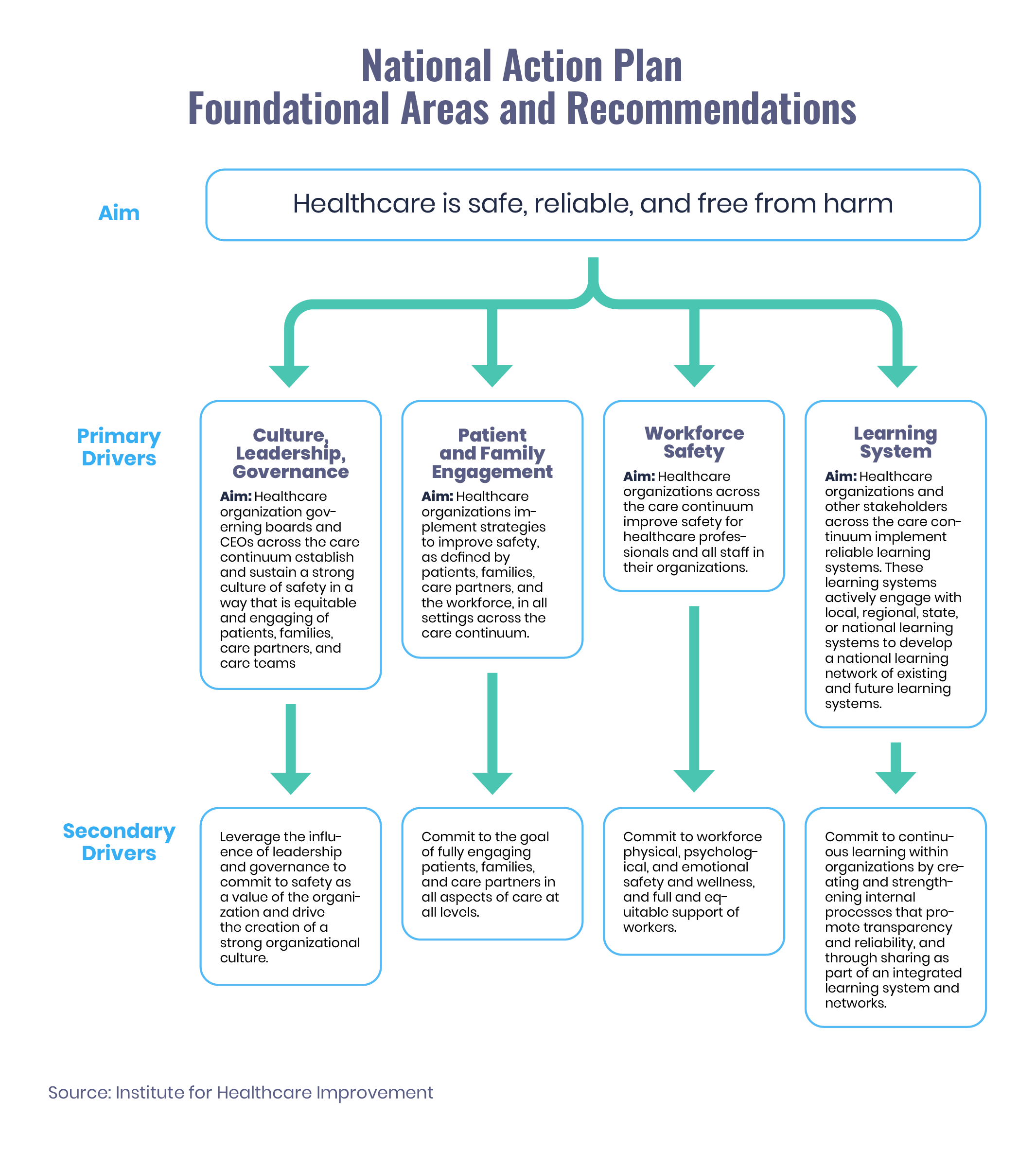
4 Foundational Areas of Total Systems Safety
The National Action Plan centers on four foundational and interdependent areas, which the NSC prioritized as essential to create total systems safety:
- Culture, Leadership, and Governance: The imperative for leaders, governance bodies, and policymakers to demonstrate and foster their deeply held professional commitments to patient safety as a core value and promote the development of cultures of safety.
- Patient and Family Engagement: The expansion of authentic patient and family engagement; the practice of co-designing and co-producing care with patients, families, and care partners to ensure their meaningful partnership in all aspects of care design, delivery, and operations.
- Workforce Safety: Ensuring safety in healthcare – including the safety of the organization and the workforce – is a prerequisite to advancing patient safety. We need to work toward a unified, total systems-based perspective and approach to eliminate patient harm and harm to the workforce.
- Learning System: Establishing networked and continuous learning; forging learning systems within and across healthcare organizations to encourage widespread sharing, learning, and improvement.
The NSC considers these areas to be fundamental because they provide a solid foundation on which broader safety initiatives can be built. Furthermore, they’re codependent because advancing in one area alone is nearly impossible without advancing in all of them.
The ensuing recommendations in these foundational areas build on the substantial body of experience, evidence, and learned lessons that the NSC has collected and will continue to evaluate as our understanding and evidence evolve in the years to come.
Culture, Leadership, and Governance
Assure that safety is a demonstrated core value. Senior leaders and governance bodies must prioritize safety as part of the organization’s mission and values and hold themselves and their organizations accountable for engagement and improvement. They must build an organizational culture that encourages trust and transparency, provides physical and psychological safety for the workforce, and supports the workforce’s joy in work.
Implementation tactic example: Implement the practices of a just culture, ensuring that policies, procedures, and performance evaluations support a safety culture, regularly assessing culture, determining the root causes of culture issues, and continually taking steps to improve culture.
Assess capabilities and commit resources to advance safety in healthcare. Governance bodies and senior leaders must regularly evaluate their personal and organizational capabilities, as well as the core competencies of all staff, to achieve sustained patient safety outcomes that are both reliable and safe.
Implementation tactic example: Identify, mitigate, and address system problems that contribute to physical, psychological, and emotional workforce harm, such as burnout, and provide appropriate resources to employees.
Share information about employee and patient safety to promote transparency. Governance bodies and senior leaders must ensure that their organizations develop, implement, and enforce standard processes to transparently share information and data about near misses, harmful incidents, and lessons learned in a timely manner, within and across their organizations, as well as with patients, families, and care partners. Additionally, processes must be established to address resourcing needs and implement solutions to mitigate patient harm.
Implementation tactic example: Share key patient and workforce safety data, stories, and contextually relevant information with board members, leaders, and all members of the care team, including health care professionals, patients, families, and care partners. Promptly inform key leaders and governance bodies of serious reportable events and the status of root cause analyses and action planning.
Implement competency-based governance and leadership. Senior leaders must ensure that quality and patient safety competencies are identified and evaluated during onboarding and throughout the tenure of governance bodies and leaders. Competencies must include the knowledge, skills, and attributes needed to champion patient safety practices that lead to measurable improvement in care.
Implementation tactic example: Use a standardized assessment to ensure that board members and senior leaders demonstrate competencies in safety, equity, and data literacy. Track progress over time in their oversight of these areas and in their use of data. Ensure that ongoing education provides coordinated guidance, curriculum, and assessment for board members and leaders across governance-support organizations.

Patient and Family Engagement
Establish competencies for all health care professionals for the engagement of patients, families, and care partners. Healthcare leaders in all care settings must ensure that healthcare professionals are prepared to form equitable and effective partnerships with patients, families, and care partners.
Implementation tactic example: Ensure that health care professionals and staff are trained to recognize and prevent unconscious bias and are competent in equitable, effective communication strategies.
Engage patients, families, and care partners in the co-production of care. Healthcare leaders and healthcare professionals need to fully engage with patients, families, and care partners in ongoing co-design and co-production of their care.
Implementation tactic example: Ensure full transparency by ensuring that patients and authorized family or care partners have timely access to a patient’s electronic health records, including visit notes, discharge summaries, and proxy access to patient portals to avoid errors, delayed diagnoses, or other safety risks.
Include patients, families, and care partners in leadership, governance, and safety and improvement efforts. Healthcare leaders and governance bodies need to involve patients, families, and care partners from all backgrounds in healthcare oversight, design, and improvement, in addition to harm reduction efforts.
Implementation tactic example: Conduct organizational assessments of the availability and effectiveness of patient and family engagement strategies and address any identified gaps.
Ensure equitable engagement for all patients, families, and care partners. To ensure the ongoing engagement of patients, families, and care partners in safety, healthcare leaders must actively and equitably partner with all patients, families, care partners, and relevant community organizations.
Implementation tactic example: Establish systems to analyze safety data to identify and address gaps related to the social determinants of health, such as being at risk for housing or food insecurity, and to share community resources that can provide support.
Promote a culture of trust and respect for patients, families, and care partners. Healthcare leaders must ensure that healthcare professionals and all personnel interact respectfully and transparently with patients, families, and care partners and with one other.
Implementation tactic example: Implement and maintain programs for providing appropriate ongoing support in the aftermath of harm. When preventable harm occurs, interview the patient and family and include them, as appropriate, in root cause analysis. Openly and honestly disclose when the standard of care is breached, apologize, address physical and psychological harm, and offer the opportunity to discuss appropriate remedies.
Workforce Safety
Implement a systems approach to workforce safety. Ensure that every healthcare organization across the care continuum has comprehensive workforce safety programs in place. Senior leaders must develop and implement governance and oversight structures to support a systems approach to employee safety, which includes leadership and engagement, safety management systems, risk reduction, and performance analytics and management.
Implementation tactic example: Engage managers and staff in preparing standardized job hazard analytics to systematically assess the hazard risks of all job tasks. Risks include ergonomic, chemical, infectious pathogens, assaults, slippery surfaces, and other conditions or activities that could result in injury or illness.
Assume accountability for physical and psychological safety and a healthy work environment that fosters the joy of the healthcare workforce. Organizational governance bodies must ensure that leaders in clinical care and operations across all care settings collaborate and are jointly accountable for the effectiveness of workforce safety programs.
Implementation tactic example: Establish an employee safety system and ensure that key safety practices, including safe patient handling, ergonomics, falls, exposure, violence prevention, and safe sharps practices, are embedded into systems, workflows, practices, and care protocols.
Develop, resource, and execute on priority programs that equitably foster and promote workforce safety. Governing bodies and senior leaders must establish and implement programs to prevent all workforce injuries. Special emphasis must be placed on the development of robust programs to prevent the injuries that are most prevalent and impactful, and programs that support psychological safety and joy in work.
Implementation tactic example: Adopt metrics and performance dashboards that are reflective of physical and psychological safety and joy in work (e.g., turnover and absentee rates, safety culture ratings, requests to reduce hours, safety culture index, staff suicide rates, likelihood to recommend organization).
Learning System
Facilitate both intra- and inter-organizational learning. All healthcare organizations must take steps to become collaborative learning organizations by using high-reliability principles, ensuring robust learning feedback loops, and engaging with established learning systems.
Implementation tactic example: Develop and implement processes to systematically learn from safety events, including input from patients, families, care partners, and health care professionals at the point of care. Integrate lessons learned into the process of setting goals and priorities for interventions to improve patient safety.
Accelerate the development of the best possible safety learning networks. Leaders of existing safety learning networks must engage in the development of a network of networks to identify and increase adoption of best practices so that, working together, all can become the most effective learning networks possible.
Implementation tactic example: Develop a national network of existing safety learning networks. Start by inviting leaders of safety learning networks to join with the aim of accelerating the pace of improvement. Through collaboration, existing networks can identify and adopt best practices for learning networks, use data analytics to identify opportunities for improvement, learn from variation across networks to improve all, and support the growth and development of network leaders and infrastructure.
Initiate and develop systems to facilitate interprofessional education and training on safety. Academic institutions, professional educators, and leading patient safety and quality organizations must collaborate to better understand how to improve safety in healthcare education and training for clinical and administrative staff. These organizations must identify and share openly all best practices on the creation, dissemination, and assessment of safety education and training methods and materials.
Implementation tactic example: Create new multidisciplinary learning networks to better understand how to improve safety education and training for clinical and administrative staff. Identify and share best practices on the creation, dissemination, and assessment of education and training methods and materials.
Develop shared goals for safety across the continuum of care. Leaders of healthcare organizations, employers, and policymakers must collaborate with leaders of safety learning networks to adopt national-level goals to eliminate specific types of harm across the continuum of care, ultimately advancing the development and dissemination of methodologies and processes to improve safety.
Implementation tactic example: Establish a national expert group to identify and prioritize specific safety issues for improvement, based on data and information from the providers of care; establish goals; identify data for measurement; determine a means for measurement; and set time-bound targets for achieving them.
Expedite industry-wide coordination, collaboration, and cooperation on safety. Modelling leaders in civil aviation, healthcare leaders representing all stakeholders must actively develop a public-private partnership to use the power of data sharing and cooperative learning to identify and solve the most urgent and emerging patient safety problems.
Implementation tactic example: Identify existing partnerships and explore funding options from governmental and non-governmental sources to convene and conduct activities. Model efforts after other industries that have successful public-private partnerships related to safety (e.g., civil aviation, nuclear power, etc.)
The healthcare community needs broad and meaningful collaboration and coordination among all stakeholders to improve safety in healthcare. Every stakeholder can play a part in advancing some or all of the recommendations in the National Action Plan.
By planning and investing together, mobilizing resources together, learning together, and sharing lessons learned, we can drive meaningful change and advance the goal of creating the safest health care for patients and those who care for them.


