What if your healthcare organization could balance accountability with fairness, creating a work environment where mistakes lead to growth rather than fear? Enter the concept of a "just culture"—a transformative approach to safety and accountability that empowers organizations to build trust while addressing system vulnerabilities and employee behaviors fairly. Embracing a just culture in healthcare ensures a safer, more transparent environment for both employees and patients alike.
What is Just Culture in Healthcare?
First introduced in the healthcare space in a 2001 report by David Marx, just culture is defined as a system of shared accountability. In a just culture, organizations are responsible for designing safe systems and responding to employee behaviors in a fair and just manner, while employees are accountable for the their decisions and for reporting safety observations and system vulnerabilities.
In a just culture, safety incidents and events aren't viewed as failures but as opportunities to identify and address system risks and organizational behaviors. It recognizes that even competent professionals can make mistakes (we're all humans after all), and that repeated or multiple incidents often point to solvable issues arising from the interaction between people and the systems in which they work.
By considering all contributing factors—human, environmental, technical, and beyond—a just culture fosters continuous improvement, and subsequently better patient safety outcomes.
What is Patient Safety?
Patient safety refers to how healthcare organizations “protect their patients from errors, injuries, accidents, and infections.”
Preventable medication errors cost approximately $20 billion annually. Effective Patient Safety programs can improve patient outcomes and reduce costs at the same time.
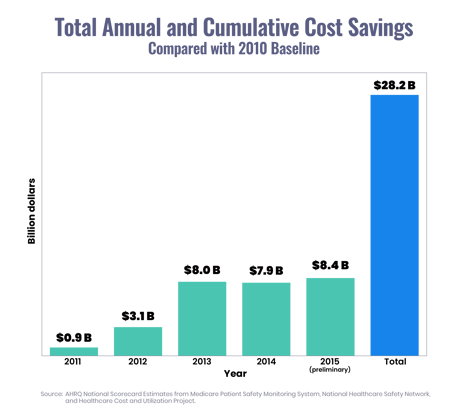
In 2015, due to an increased focus on patient safety, it is estimated that 125,000 fewer patients died in the hospital as a result of hospital-acquired infections (HACs). Not only that– approximately $28 billion in health care costs were saved, as well.
Nevertheless, as of 2024, it's estimated that around 400,000 hospitalized patients annually suffer from preventable harm. Additionally, medical errors are costing approximately $20 billion each year. Given these numbers, it's clear that patient safety must remain a paramount concern and responsibility for every healthcare professional. There is still significant progress to be made in this area.
What is a Patient Safety Culture in Healthcare?
Patient safety culture is the culmination “of individual and group beliefs, values, attitudes, perceptions, competencies, and patterns of behavior that determine the organization’s commitment to quality and patient safety.”
Essentially, a “patient safety culture” means that every member of a healthcare team is equally committed to putting patient safety first, and they continuously engage in actions that reflect that commitment. This culture is also one that is Just and encourages all members of a team to report harmful incidents and wrongdoings without fear of retaliation.
10 Elements of a Just Culture in Healthcare
Is your healthcare organization committed to patient safety? If so, here are ten key elements of a Just Culture that you and your team should be aware of:
1. Use a Transparent Approach
Use a transparent, non-punitive approach to report and learn from incidents, close calls and unsafe conditions. (2) An increase in the number of incidents reported and effective reporting by all team members leads to improved patient outcomes and helps drive overall organizational change.
This approach includes encouragement of collaboration across all ranks and disciplines to seek solutions to patient safety problems.
2. Define Set Processes
Use clear, just, and transparent risk-based processes for recognizing and distinguishing human errors and system errors from unsafe actions. The goal of every team member is Zero Harm to patients. In order to achieve Zero Harm, patient safety must be embedded into the organizational culture. (2, 5)
3. Lead by Example
In a true patient safety culture, all organizational leaders are expected to adopt and lead by example. When leaders display the appropriate behaviors, they can decrease feelings of intimidation and increase the probability of their staff reporting errors and safety concerns. (2)
Promoting a culture of safety is the responsibility of everyone in the organization, whether they are leaders, frontline staff, contract personnel or volunteers.
4. Put Policies in Place
Organizations are expected to create and adhere to policies that support their safety culture. This means setting up systems and policies around the reporting of adverse events, near misses and unsafe conditions that can lead to further patient injuries. Policies must be enforced, communicated and made easily accessible to all team members within the organization. (2)
5. Focus on shared accountability
The Patient Safety Culture should also be a Just Culture, one which recognizes all team members who report incidents, events and near misses. Wrongdoings are almost always the result of system failures; therefore, blame should not be placed on individuals.
A Just Culture nursing also recognizes those who identify unsafe conditions, or who have good suggestions for patient safety improvements.
It is important that leadership shares information brought forward regarding these incidents, near misses and recommendations for safety improvements with all team members so all can learn from these “free lessons”. (2, 3)
6. Use Validated Tools
The next important element to improve patient safety culture is to use validated tools to measure patient safety. An organization is expected to determine a baseline measurement on their safety culture performance using a validated tool. Two commonly used tools are AHRQ's Patient Safety Culture Surveys and the Safety Attitudes Questionnaire. AHRQ provides annual updated benchmarking data from the hospital survey.
There is an expectation that healthcare institutions repeat organizational assessment of their safety culture every 18 to 24 months in order to review progress and sustain improvements. (2, 4)
7. Act on the Data
Safety culture survey results are to be analyzed from all departments to find opportunities for quality and safety improvement. Across the country, there is documented evidence of considerable variation in perceptions of safety culture across organizations and job descriptions. Understanding these variations in perceptions is valuable to the organization in developing and implementing interventions to comprehensibly address safety concerns.(2, 4)
8. Commit the Necessary Resources
Organizations must commit resources to address any patient safety concerns that arise from analysis of safety culture surveys. These resources might take the form of personnel, additional training, or increased funding.
Funding is often necessary in order to develop and implement interventions that increase patient safety at the site of care. (2, 4)
9. Train Your Team
Safety culture team training is embedded into quality improvement and risk management projects and organizational processes to strengthen safety systems. An effective Just Culture healthcare encourages collaboration across ranks and disciplines to seek solutions to patient safety problems.
10. Regularly Assess Strengths and Weaknesses
Organizations must proactively assess system strengths and vulnerabilities, and prioritize them for enhancement or improvement.
Historically, healthcare organizations have approached patient safety as a reaction to an incident that harmed a patient.
A proactive incident reporting approach is to search for potential breakdowns in safety and address those potential breakdowns in order to consistently ensure patient safety. (2, 6)
What is a just culture in healthcare? How does your healthcare organization strive to incorporate patient safety into your culture? If you're looking to improve patient safety outcomes, a strong incident reporting system is a great place to start.
Trudi Stafford, PhD, RN, and Clinical Advisor at PHP shares insight on developing a just patient safety culture.
Trudi Stafford has 30+ years of health care leadership experience with an emphasis on informatics to positively impact patient safety and health care quality. She is a doctorally-prepared nurse executive with prior work experience as the Chief Nursing Officer at three of the nation’s largest health systems.
References
- The Patient Safety Systems (PS) chapter of The Joint Commission Accreditation Manual. Retrieved on August 3, 2019 at https://www.jointcommission.org/patient_safety_systems_chapter_for_the_hospital_program/
- 11 Tenets of a Safety Culture, The Joint Commission. Retrieved on August 3, 2019 at https://www.jointcommission.org/assets/1/6/SEA_57_infographic_11_tenets_safety_culture.pdf
- Joint Commission Outlines 11 Tenets of a Safety Culture, Risk Management News. Retrieved on August 3, 2019 at https://www.ecri.org/components/HRCAlerts/Pages/HRCAlerts030817_Joint.aspx
- Culture of Safety. Patient Safety Network. Agency for Healthcare Research and Quality. Retrieved on August 2, 2019 at https://psnet.ahrq.gov/primers/primer/5/Culture-of-Safety
- Source not available
- Safer Clinical Systems: A new, proactive approach to building safe healthcare systems. Warwick Medical School. Retrieved on August 3, 2019 at http://patientsafety.health.org.uk/sites/default/files/resources/hf_safer_clinical_systems_reference_guide_final_1.pdf
- What is Patient Safety. Leapfrog Hospital Safety Grade. Retrieved on August 3, 2019 at https://www.hospitalsafetygrade.org/what-is-patient-safety
- Weaver, SJ, Lubomksi, LH, Wilson RF, Pioh, ER, Martinez, KA, and Dy, SM. (2016) Promoting a Culture of Safety as a Patient Safety Strategy: A Systematic Review. Ann Intern Med. Retrieved on August 3, 2019 at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4710092/
- What is CANDOR? MedStar Health Institute for Quality and Safety. Retrieved on August 3, 2019 at https://www.medstariqs.org/centers-of-expertise/center-for-open-honest-communication/what-is-candor/
- Mayer, D. (Presentation). CANDOR: The Integration of Transparency, High Reliability, Human Factors, and Patient/Family Partnerships in Changing a Safety Culture. Presentation
- 2018 Hospital SOPS Database Report Executive Summary Infographic. Agency for Healthcare Research and Quality. Retrieved on August 3, 2019 at https://www.ahrq.gov/sites/default/files/wysiwyg/sops/quality-patient-safety/patientsafetyculture/2018hospitalsopsrptexecsum_0.pdf
- Hospital-Acquired Conditions 2010 to 2015: Interim Data From National Efforts to Make Health Care Safer.Agency for Healthcare Research and Quality. Retrieved on August 4, 2019 at https://www.ahrq.gov/professionals/quality-patient-safety/pfp/2015-interim.html?utm_source=AHRQ&utm_medium=PR&utm_term=&utm_content=6&utm_campaign=AHRQ_NSOHAC_2016#exhibit1



